Our Proven Implementation Process
We’ve developed the ClinicDesk Implementation Framework™, a proven, step-by-step system for deploying AI medical coding safely, accurately, and seamlessly within your clinic’s clinical workflow.
Discovery Call
We begin by understanding your clinic’s specialty, workflows, payer mix, and current coding process. This includes reviewing encounter volume, documentation habits, common procedures, and where time or revenue is being lost today. The goal is to configure ClinicDesk around how your clinic actually operates—not force you to change how you practice.
Compliance
Before any data is processed, we establish the compliance foundation. This includes HIPAA alignment, security controls, access roles, audit logging requirements, and signing a Business Associate Agreements (BAAs). Compliance is treated as a prerequisite- not an afterthought.

EHR Connection
We integrate ClinicDesk with all major EHR systems, including athenahealth, to ensure data flows seamlessly between your EHR and ClinicDesk. This connection is designed to require minimal change to your existing clinical workflow—providers and staff continue working in the systems they already know, while ClinicDesk works quietly in the background to support accurate medical coding.

Coding Rules Build-out
ClinicDesk is configured with coding logic tailored to your specialty, payer requirements, and clinic-specific preferences. This includes CPT, HCPCS, ICD-10-CM, modifiers, and documentation rules aligned to how your providers document care—helping ensure coding accuracy without forcing extra work on your team.
If you have someone on your staff (even part time) that helps with your clinic’s billing, they will be who we work with most in this phase. By the end of this phase, you’ll start to see that person’s workload cut in half.
QA Testing
Before going live, we run ClinicDesk in parallel with your existing coding workflow. Outputs are validated against historical claims, internal benchmarks, and edge cases to ensure accuracy, consistency, and defensibility. We get an apples-to-apples comparison of what your claims would look like before and after going through your ClinicDesk workflow and improve any opportunities we find to make it even better. This phase is focused on confidence and correctness.

Staff Training
We provide role-based training tailored to your clinic’s size and structure. Training differs for providers who previously handled their own coding versus clinics with dedicated billing or coding staff. Administrators receive a separate training session focused on ClinicDesk’s administrative settings, reporting, and oversight tools. The goal is to ensure every role knows exactly how ClinicDesk fits into their responsibilities—without added complexity.
We record your training sessions and link them in your account so you can re-watch them anytime. Your recordings are also great for training future staff in less than 1 hour.
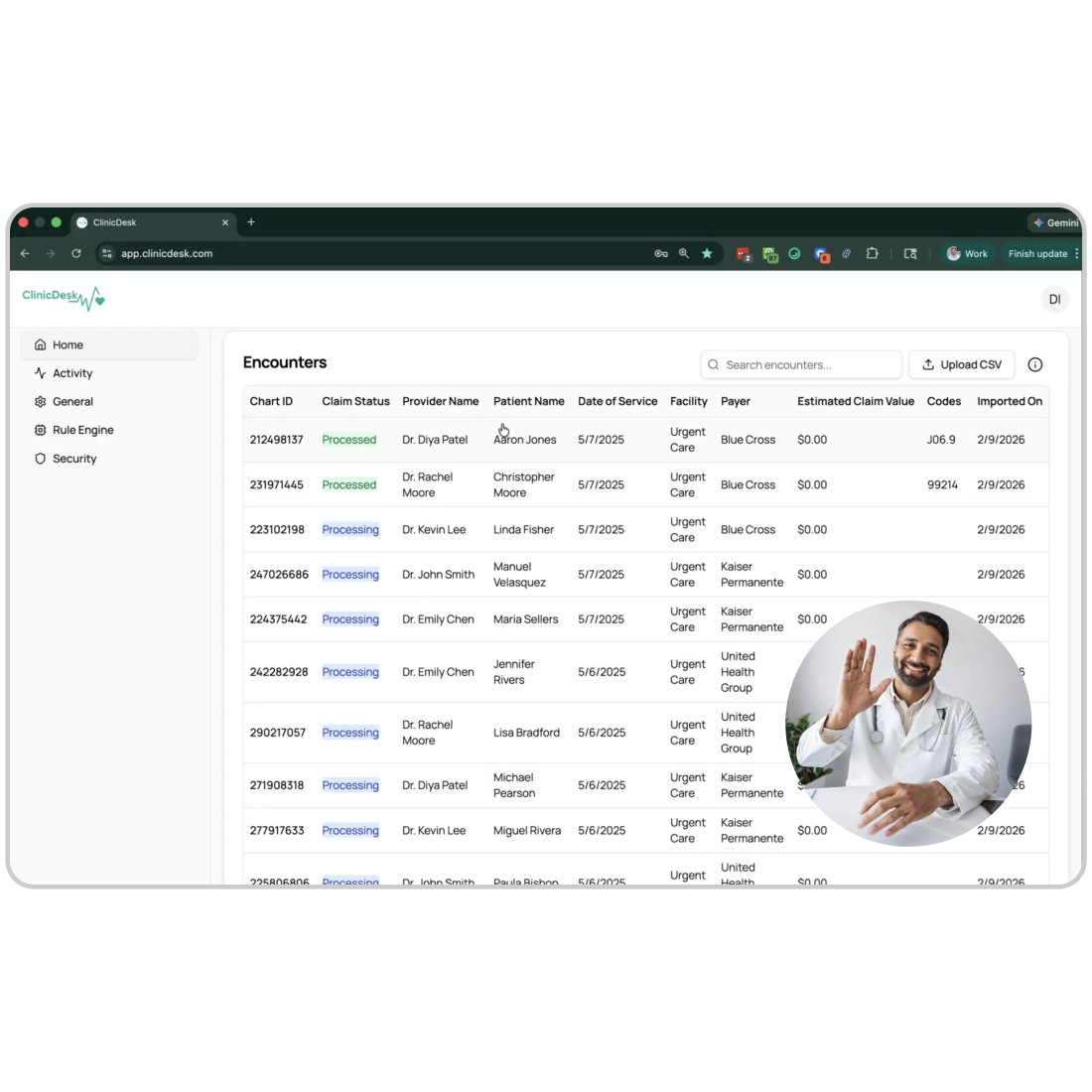
Go-Live Day
Once everything is validated, ClinicDesk is introduced into your clinical workflow.
For most providers, this change is barely noticeable—ClinicDesk runs silently in the background while you focus on patient care. You’ll spend less time documenting and worrying about coding details in your EHR, while accuracy and efficiency improve overnight behind the scenes.
For billers, over 72% of your workload gets eliminated overnight by the automations you helped set up in your Rules Engine. This frees up your time to focus on holding Payers accountable, increasing collection rates, and fighting back Payer disputes easily using your ClinicDesk Audit Trail PDF exportable reports.
For administrators, you’ll start seeing revenue improve by billing for what you deserve. Watch your clinic’s RVUs increase by billing for codes previously missed, fixing your upcoding and downcoding automatically, and enjoy your rejection and denial rates plummet. Use your improved RAF Scores to negotiate better rates in your Payer contracts and export data reports from ClinicDesk to show your improved HCC, HEDIS, and VBP analytics.

Ongoing Performance Reporting & Support
After your Go-Live, we continue to monitor performance, update coding logic as regulations evolve, and support your team as volumes grow. ClinicDesk improves over time—adapting to new payers, new procedures, and new operational realities—so your clinic stays ahead and compliant.
Watch your revenue grow as your new Medical Coding AI correctly codes and bills for the services your team is actually delivering. Get paid what you deserve while serving the exact same patients and providing the exact same care as you are now- while spending less time documenting it.


